For much of human history, aging meant losing teeth. Many historical portraits feature subjects, stoic and unsmiling, doing their best to hide decaying teeth. Thanks to advances in dentistry and public health, those days are largely over. For Americans, edentulism, or the complete loss of teeth, is no longer considered inevitable, and most today can expect to keep their teeth for a lifetime.
Despite those developments, significant room for improvement remains. The Centers for Disease Control and Prevention found that between 2009 and 2014, about 40 percent of American adults 30 years or older, and 60 percent of Americans over 65, had some form of periodontitis, a severe inflammation of the gums resulting from tooth decay.
The issue extends far beyond oral hygiene. As dentists and researchers uncover the links between oral health and chronic disease, they’re finding that the healthier the teeth and gums, the healthier the body. For longer, better lives, the state of our teeth and gums deserves a closer look.
Gateway to health
At its root, periodontal disease is an inflammatory condition. The invasion of anaerobic bacteria at the junction of tooth and bone unleashes a cascade of immune responses. When oral bacteria enter the system, through either an airway or a wound, they can fuel further inflammation.
Research in recent decades has demonstrated links between poor oral health and diabetes, heart disease, autoimmune disorders and even dementia—all of which are suspected to be inflammatory diseases. This makes sense. The surface area of oral tissue is roughly equivalent in size to the palm of a hand. Inflammation over such an area has been shown to worsen the effects of high sugar in diabetes and damage the endothelium of arteries in vascular disease. Periodontal treatment is known to reduce levels of inflammatory markers in the blood, such as C-reactive protein.
Inflammation is not the only way that oral health impacts health. A systematic review found 15 studies that demonstrated that daily toothbrushing decreases the incidence of death among patients admitted to the intensive care unit, most likely by preventing bacteria from the mouth from traveling into the lungs. Older adults without teeth are more likely to have depression and report social isolation, because having teeth allows us to speak well and participate more fully in community. Studies have found lower levels of iron and vitamins A and C in the blood of older adults with dentures, because these nutrients are typically found in nutrient-dense foods like meat and vegetables, both of which can be difficult to chew.
Teeth even play a role in financial security and success. A study by economists Sherri Glied and Matthew Neidell found that women from low-income families who grew up in counties with water fluoridation earned wages that were 4 percent higher than those without fluoride access. The authors excluded factors such as these groups choosing different jobs or being more or less productive than each other. They concluded the wage difference was largely because the subjects’ healthier smiles meant that employers (and, presumably, tipping customers) preferred them.
Golden age of dentistry
In the past two decades, dentistry has made remarkable technological advances. Tooth-colored composite materials can make fillings nearly invisible; they survive longer in the mouth with less risk of new decay and require the removal of less healthy tooth structure than older materials. Crowns can be color-matched using artificial intelligence and fit with a custom scan. The first human trial of a drug to regrow a lost tooth began in September 2024. Scientists are developing a caries vaccine that could target Streptococcus mutans, the bacteria most responsible for dental decay.
Patients can now receive a crown produced from 3D mouth scans within the same day as their visit. Instead of having to be anesthetized in an operating room, very young children can have their cavities arrested completely with a thin coat of silver diamine fluoride, which could soon be used in nursing homes, rehab facilities and even doctors’ offices.
Dental implants have revolutionized tooth replacement by providing a natural-looking tooth that is fully integrated with the jawbone. For people missing all their teeth, dentures attached to just two implants in the lower jaw can dramatically improve the ability to chew while also making the denture look more natural. In the future, lab-grown teeth may offer a biological replacement that could fully restore a smile.
The question today is, How can we ensure that good dental care reaches everyone?
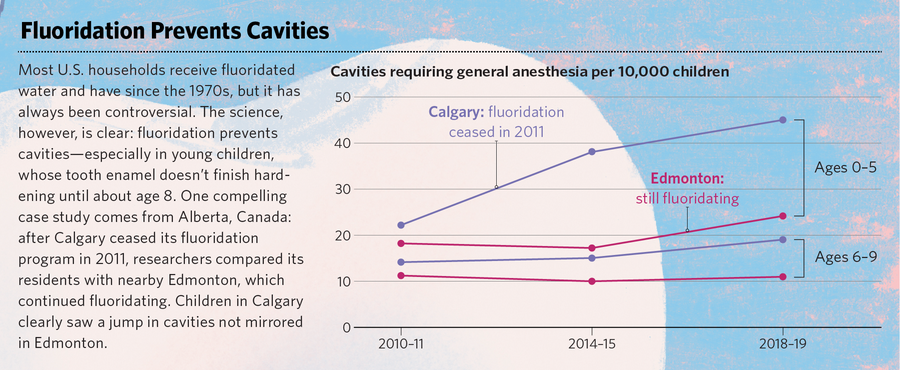
Graphic by Katie Peek; Illustration by @mattiariami/Salzmanart.com; Source: Yazdanbakhsh et al., “Community water fluoride cessation and rate of caries-related pediatric dental treatments under general anesthesia in Alberta, Canada,” Canadian Journal of Public Health, February 2024
A mandate for health
Dental problems used to be more prevalent among the wealthy than the poor, mainly because the rich had greater access to sugar, which promotes tooth decay. George Washington had multiple pairs of dentures over the course of his life. While it would be unthinkable for a U.S. president today to lack teeth, vulnerable populations such as low-income, rural and marginalized older adults are now far more likely to experience tooth loss. These individuals often face barriers to dental care throughout their lives, from childhood toothaches that kept them out of school, to jobs that did not offer dental insurance.
Compounding these issues, Medicare, the primary insurer for Americans over 65, does not cover routine dental care. A statute in the Social Security Act implemented in 1965 blocks Medicare from covering dental care. My research shows a nearly five-percentage-point increase in missing teeth once individuals lose access to employer-sponsored dental insurance and enroll in Medicare. Today, only about half of adults over 65 visit a dentist annually. President Joe Biden proposed a Medicare dental benefit in his 2021 Build Back Better bill, but it was removed before the legislation passed; subsequent efforts have stalled.
To ensure everyone benefits, dental care must be accessible from childhood onward. Evidence-based strategies to improve oral health include increasing the number of dentists who accept Medicaid, expanding the types of dental services it covers and adding more dental therapists—professionals similar to nurse practitioners—to the workforce.
Fewer than a third of dentists accept Medicaid, the primary insurance for low-income Americans. In many states, Medicaid offers limited or no dental coverage for adults. The rural dentist workforce, like the rural workforce in general, is aging, and younger dentists are more likely to practice in urban and suburban areas.
Even community water fluoridation, the bedrock of dental public health, has come under attack because of concerns about neurotoxicity, even though fluoride in public-water supplies is far below dangerous levels. Fluoridation, which strengthens children’s teeth as they form and continues to prevent cavities in adulthood, accounts for much of the progress made in oral health during the 20th century; the baby boomer generation was the first to benefit from fluoride in their water during childhood. Today, many rural communities still rely on well water or other decentralized water sources, which have never been fluoridated.
In the end, the future of oral health may depend less on cutting-edge innovations and more on ensuring that the basics—such as access to fluoride, routine dental care and affordable treatments—are available to everyone. Our smiles, and our healthspans, could depend on it.
Explore the emerging science of healthspan in other stories in this special report.
link

